 consider hyperkalaemia, hypocalcaemia or cardiotoxicity.treat the cause of obstructive shock, administer fluids and inopressors.tamponade, tension, dynamic hyperinflation or PE) or underfilling (e.g. early echocardiography, provides additional information regarding intravascular volume status (ventricular volume), cardiac tamponade, mass lesions (tumour, clot), left ventricular contractility and regional wall motion.early arterial line placement and ETCO2 monitoring.Survival upon hospital discharge and after 180 days occurred only in patients in pseudo-EMD (22.2% and 14.8%, respectively).rates of ROSC were 70.4% for those in pseudo-EMD, 20.0% for those in EMD, and 23.5% for those in asystole.94% of patients received ROSC and 50% had good neurological outcomes.These patients were administered vasopressin (an additional vasopressor) and had CPR ceased for 15 seconds.in a small trial, ETCO2 and echocardiography were used to confirm pseudo-PEA.Pseudo-PEA is associated with better outcomes than true EMD raised mean intrathoracic pressure due to chest compression can be expected to reduce rather than to increase cardiac filling.In animal models asynchronous CPR during pseudo-PEA is harmful.echocardiography or Doppler ultrasound demonstrating cardiac pulsatility.high ETCO2 readings in intubated patients.arterial line placement during cardiac arrest (identified by the presence of a blood pressure).Pseudo-PEA can be detected in the absence of a palpable pulse by:.Pseudo-PEA is essentially a severe shock state and is distinct from true electro-mechanical dissociation Weiser et al (2018) found that the >60/min group showed a 30-days-survival rate of 22% and a good neurological outcome in 15% of all patients in Vienna, Austria.Step 1: Determine if the PEA is narrow (QRS duration 60/min may have better outcomes, comparable to OOHCA patients with shockable rhythms.The Littman algorithm use ECG waveform and echo findings to help stratify likely causes (Littman et al, 2014): However, this list is incomplete – for instance, non-ischemic cardiac disorders and intracranial haemorrhage occurred in 8.3% and 6.9% of PEA cases (Beun et al, 2015) Hyper/hypokalaemia and metabolic disorders.The causes of PEA are widely thought of as the 4Hs and 4Ts 
In Victoria, Australia, ~12% of OOHCA with a non-shockable rhythm is PEA (the majority are asystole).Need to seek and treat the underlying cause.Overall, prognosis of PEA far less favourable than VF/VT, prognosis for out-of-hospital cardiac arrests (OOHCA) with initial asystole or pulseless electrical activity is 60/min and ‘pseudo-PEA’. 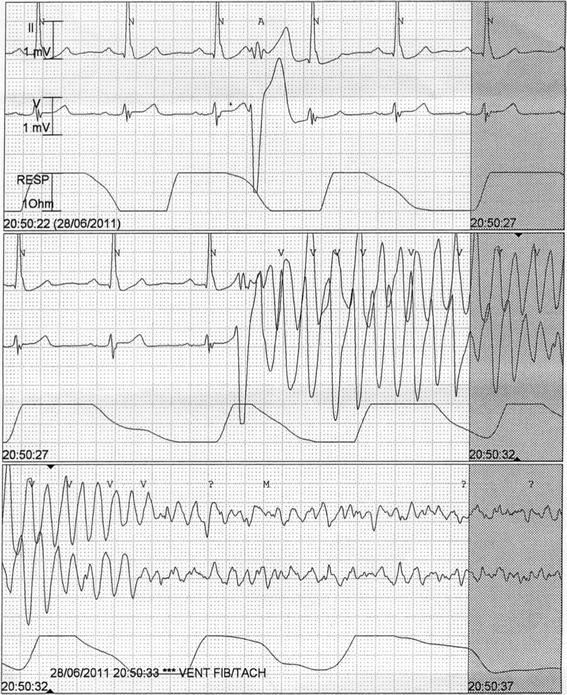
The ‘one size fits all’ approach of current ALS algorithms may be inappropriate given the heterogeneity of PEA states.In reality, pulseless electrical activity encompasses a very heterogeneous variety of severe circulatory shock states ranging in severity from pseudo-cardiac arrest to true electro-mechanical dissociation with cardiac standstill. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
